top of page
Between business and personal life
Our Blog


The Full Mouth Falcon
Full-arch rehabilitation with Falcon navigation showed impressive real-time control of angulation, depth, and implant positioning, especially in complex anatomy. However, limitations emerged: marker interference, tracking instability, calibration time, and loss of global parallelism. Falcon enhances local precision, but in full-arch cases, it may compromise overall control.
Apr 309 min read

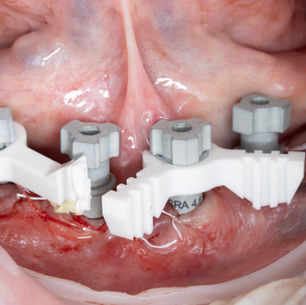
The New 4mm (2.0 Version)
This week we pushed the limits of what is surgically possible. Using a new 4 mm implant, we treated a severely atrophic mandible without grafting, relying on precision, anatomy, and decision-making under pressure. This was not about short implants — it was about control, responsibility, and executing when there is no margin for error.
Apr 254 min read


When Your Mind Says Stop — But You Go Anyway
Success is not just about working hard — it’s about acting despite discomfort. The mind resists uncertainty, but growth happens when you move anyway. Like climbing, you don’t know if you’ll reach the top until you start. You may succeed or fail, but doing nothing guarantees the outcome. The only route that truly fails… is the one you never climb.
Apr 193 min read


When Biomechanics Catches Up
This case report describes a delayed prosthetic failure more than 10 years after mandibular full-arch rehabilitation with limited AP spread. Initially stable under low functional load, the system failed following maxillary fixed rehabilitation, increasing occlusal forces. Failure occurred at the prosthetic interface, highlighting the long-term impact of compromised biomechanics.
Apr 124 min read


The easy Açai !!!
Two patients. Same symptom: a moving crown. Completely different biology. One ideal immediate implant case with high stability; the other a compromised indication that failed. At two weeks, true implant loss is unlikely. The issue? Mechanical, not biological. In implant dentistry, not everything that moves is lost — but clarity in diagnosis is everything.
Apr 33 min read

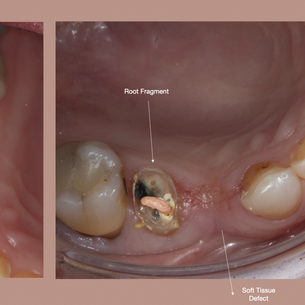
Read the Canine - Dont Hit him
“Most upper 1st premolar implant mistakes don’t come from lack of skill — they come from not reading the canine.” Good morning, ChatGPT. Good morning, world. Good morning, Lisbon. Today we’re finally hitting 25°C. Real spring. I just finished an amazing climbing session — one more step toward conquering my 6C+ . Today I fell on a move I had never reached before. It was a nice feeling because a lot of people was watching and i´m baby steps to close the 6 deal and move to the 7
Mar 294 min read


🦷 Immediate loading is not about speed — it’s about control
Full-arch rehabilitation begins long before the implant. Ridge reduction, palatal positioning, and tissue control—turning a compromised anatomy into predictable outcomes.
Mar 243 min read


Implant dentistry is a state of mind.
Climbing and dentistry share the same foundation: focus, control, and the pursuit of inner strength. Both demand precision under pressure, where small decisions redefine outcomes. Success is not accidental—it is built through awareness, adaptability, and the ability to constantly shift the equation in your favour, even when conditions are far from ideal.
Mar 222 min read

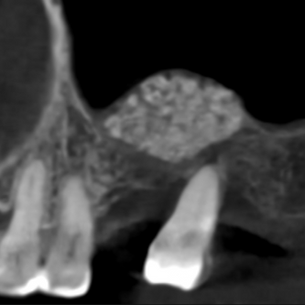
🌱 Spring, mistakes, and redemption — an implant that insisted on teaching
“We don’t notice the moment we make the wrong decision — only the moment it comes back to teach us.”
Mar 213 min read


🐻 They Die of Shame
Inspired by The Edge, this reflection explores how people don’t fail because of problems—but because they freeze in shame. In business and surgery alike, success comes from shifting instantly from error to action. Not “why did this happen?” but “what do we do next?”
Mar 162 min read
Two Sinuses, One Surgeon, One Variable
“In implant surgery, biology is constant — but humans are variable.” andré chen This week brought an interesting clinical reflection. I was waiting for the local supermarket Aucham to open this morning here in Benfica neighborhood,,, when I started thinking about a case we performed this week: a sinus elevation in the region of tooth #16. The CBCT clearly showed a severely pneumatized maxillary sinus and almost no residual bone. The patient, interestingly, had no idea this wa
Mar 83 min read

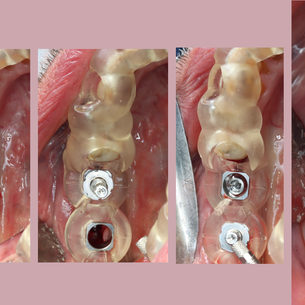
The Mandible Illusion
Posterior mandibular implantology often deceives: CBCT suggests abundant bone, yet lingual concavities and ridge atrophy reduce true volume. Guided surgery performs well in ideal conditions but may fail when drills deflect in dense or thin bone. Success depends on anatomical awareness, prosthetic-driven positioning, and intraoperative adaptability—not on the guide alone.
Mar 74 min read


🥋 Too Many Mind- The Day Surgery Stopped Being Rational The Neurobiology of Surgical Presence
When surgery deviates from plan, the greatest risk is not technical—it is mental noise. In moments of pressure, the mind can fragment or integrate. This reflection explores “Mushin”—a state where analysis fades and trained instinct takes over. Not improvisation, but deep integration. Where focus narrows, time slows, and execution becomes precise.
Mar 54 min read


When Implantology Fails the Patient
Lisbon, 00:30. After a long surgical week, one case stayed with me. A full-arch done 6 months ago—four implants in the pre-maxilla, outside bone, inflamed, failing. Not biology. Concept. We removed everything, rebuilt with proper anchorage and prosthetic logic. The patient trusted twice. Implantology didn’t fail today—decisions did.
Feb 284 min read


You Can’t Restore an Implant Like a Tooth.
"Every implant we place is a biological decision. Every crown we design is a mechanical consequence of that decision. In this case, we intentionally chose a supracrestal strategy to protect marginal bone and move the microgap away from the osseous envelope. Biologically sound. Predictable. Controlled. But biology always sends the invoice to prosthetics. When we reduce prosthetic space, we increase design responsibility. And that is where many restorations fail — not because t
Feb 175 min read


Supracrestal Ceramic Implant Placement as a Soft Tissue–Driven Alternative to Horizontal Regeneration in the Posterior Maxilla: A Case-Based Rationale
Posterior maxillary implant rehabilitation often requires augmentation due to ridge collapse and soft tissue deficiency. This case shows how supracrestal ceramic implant placement, combined with soft tissue repositioning, can be a minimally invasive alternative when grafting is not accepted. If the implant remains within the four bony walls, stable peri-implant tissues and functional outcomes may be achieved without extensive regeneration.
Feb 43 min read
Subcrestal, Supracrestal, and One-Piece Implant Placement in the Posterior Mandible
A Prosthetically Driven Concept and the Importance of Three-Dimensional Accuracy The Dream of the Supracrestal Implant Four approaches. Four levels of precision. This morning I woke up with one of those thoughts that doesn’t come from reading a paper… It comes from living implant dentistry. I slept well.Body Battery: 100% .Sleep Score: 95% . And maybe because of that… I dreamed about implants. Not an abstract dream.A surgical dream.A prosthetic dream. And the message was simp
Feb 45 min read


When the Body Hurts… But the Surgery Still Flows
Some days the body breaks… but the surgery still teaches.
A posterior implant case where restraint, soft tissue intelligence, and keratinized mucosa repositioning replaced unnecessary reconstruction.
Because true mastery is simple: you tailor the technique to the patient — not the patient to the technique.
Feb 33 min read


Margarida’s First IEXCEL Case — When the Guide Doesn’t Move
This post describes a first clinical experience with Straumann IEXCel and TLX implants placed under static guidance using the iGUIDE system.
A stepwise drilling protocol combined with dual-pin fixation provided high guide stability, predictable osteotomy preparation, and excellent primary stability.
Three posterior implants were successfully inserted with minimal deviation, highlighting the importance of method, teamwork, and precise guided workflows.
Jan 314 min read


When the Ridge is a Knife Edge… and We Still Achieve a Perfect Implant
From a knife-edge ridge to a stable foundation — all in one surgery.
Because implantology is not about adding steps… it’s about reading the bone and choosing the right architecture.
Jan 314 min read
bottom of page