When Peri-Implantitis Becomes Osteomyelitis
- Andre Chen

- 2 days ago
- 3 min read
Basel is now behind me, but Lisbon welcomed me back with that almost cinematic May atmosphere: rain falling endlessly, traffic frozen on Avenida da República, dark skies, and the strange feeling that winter never really left. Somehow, that gloomy setting perfectly matched one of the most impressive clinical cases I have seen in recent years.
About two months ago, Jenny, from Madeira, sent me a CBCT scan of a patient carrying six mandibular implants that had been placed more than twenty years ago. At first glance, the problem seemed relatively straightforward: pain, mobility of the prosthesis, and clear inflammatory signs around the implants. But the moment I looked at the scan, it became obvious that this was no longer “just” peri-implantitis.
All implants presented severe bone loss. Some of them — particularly in the regions of the 33, 34, and 35 — were practically floating inside connective tissue, with no real osteointegration left. There was no biomechanics anymore, only infected titanium surrounded by heavily compromised bone.
My recommendation was immediate:
all implants had to be removed.
But the story rapidly evolved into something much more serious.
Before surgery could even take place, the patient developed an extensive sublingual fistula and ended up hospitalized. The photograph she sent us showed a dramatic infection, clearly beyond the spectrum of conventional peri-implantitis. And here lies an important reflection: she was treated with high-dose antibiotics, but the source of the infection was never removed.
The consequence was treated.
Not the cause.
The fistula temporarily closed, but one week later the swelling returned. Jenny then removed the prosthesis together with the implants that already exhibited mobility. However, two implants remained in the mouth — especially the 44, located close to the mental foramen — because they still retained partial integration, and aggressive removal at that moment carried significant surgical risk.
When the patient arrived in Lisbon, the situation was evident. The scar left by the extraoral fistula was still clearly visible in the submandibular area, and the infection had become active again. She arrived medicated with amoxicillin and metronidazole, attempting microbiological control, particularly targeting gram-negative anaerobes.
But the real shock came when we repeated the CBCT.
The radiographic pattern no longer resembled advanced peri-implantitis alone. There was a diffuse reticulated pattern of mandibular bone destruction compatible with osteomyelitis — something that, honestly, I had rarely seen with this magnitude associated with dental implants.
At that moment, the entire surgical strategy changed.
Because removing implants in a mandible weakened by osteomyelitis is not simply a matter of reverse torque.
It is a matter of preventing a mandibular fracture.
The implant removal system had to be used with extreme caution. The classic mistake in these situations is relying purely on reverse torque extraction. But when extensive bone destruction exists, excessive force can transform a relatively controlled procedure into a catastrophic complication.
Our approach therefore became more biological and more conservative:
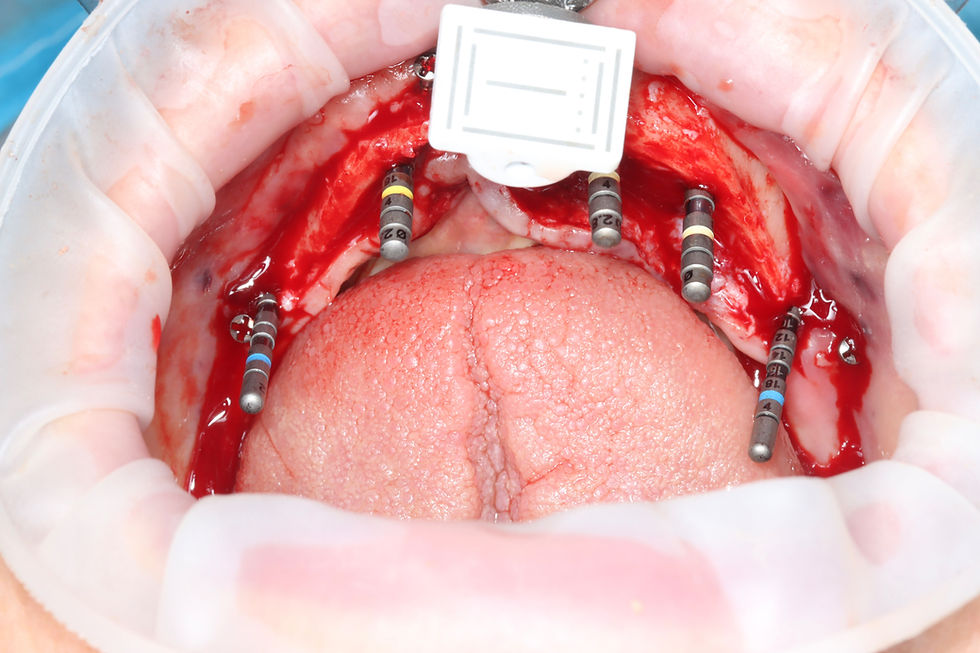
a full-thickness mucoperiosteal flap, identification and protection of the mental nerve, selective removal of residual bone around the remaining osteointegrated portions using trephines and diamond burs, and only then controlled use of the implant extractor, always maintaining torque values below approximately 35–40 Ncm.
There was another important detail.
Not all titanium behaves the same way.
The implants were Nobel Biocare Noble Replace Select implants, trilobe connection, manufactured in grade IV titanium. This matters because older grade IV titanium platforms carry a greater risk of deformation or fracture under high reverse torque forces. If the platform fractures internally, the extractor loses engagement and the surgery can rapidly become a technical nightmare.
So once again:
less force, more biology.
The surgery went well. We managed to remove the remaining implants without fracturing the mandible, performed closure with Vicryl sutures, and kept the patient in Lisbon for three days under close postoperative observation.
Now comes the most difficult phase:
waiting.
In these situations, bone requires time — a lot of time. Probably at least one year before we can properly evaluate whether sufficient healing exists to even consider a new implant-supported rehabilitation.
Until then, the patient will need to wear a removable mandibular prosthesis, which is rarely the most comfortable solution. But there are moments when priorities must be reset.
First health.
Then function.
Only afterwards sophistication.
This case left me with a powerful reflection: modern implant dentistry often speaks endlessly about connections, surfaces, dynamic navigation, and digital workflows… yet sometimes we forget that an untreated infection still obeys the same biological rules it did fifty years ago.
Bone does not read marketing.
Bone reacts to infection.
And when biology loses its balance, even implants that functioned successfully for more than twenty years can evolve into a potentially devastating condition.
This case will certainly have future chapters.
And I suspect it still has much more to teach us.
Comments