Three Implants, One Afternoon, and a Completely Different Plan
- Andre Chen

- 4 hours ago
- 4 min read
Yesterday we had one of those cases that reminds us why implant dentistry continues to be such a challenging and fascinating field. A patient referred from England arrived at the clinic with a complete prosthetic collapse in the first quadrant. She had an upper bridge supported by a canine and a first molar, but both abutments eventually failed, the bridge fractured at the pontic, and suddenly she was left with virtually no support between the canine and the molar.
The initial treatment plan had already been established. A few months earlier we had performed a sinus lift in the second quadrant, and the idea was to rehabilitate both sides with implants in the 24–25 and 14–15 areas. However, the entire case changed once we realized that tooth 13 was no longer restorable.
The first priority was to determine whether the canine could still be saved. The canine is a strategic tooth, and in most situations it is worth fighting for. But both the radiograph and the CBCT revealed a very unfavorable situation: remnants of a periapical lesion, probable ankylosis, a very difficult retreatment scenario, and above all, catastrophic coronal destruction. The decay was so extensive that attempting to restore the tooth would probably have left us holding only the root.
At that point, the treatment plan had to evolve in real time.
Originally, the idea was to place submerged implants in positions 14 and 15 and use a provisional bridge supported between the canine and the molar. But once tooth 13 became part of the extraction plan, everything changed. The CBCT clearly showed excellent palatal bone availability for anchoring a 12 mm implant, and we decided to take a more ambitious approach: if we achieved sufficient primary stability in all three implants, we would immediately proceed with a fixed provisional restoration under immediate loading.
The patient’s occlusal situation also favored this approach. She had no lower opposing teeth, which significantly reduced the functional load on the provisional prosthesis.
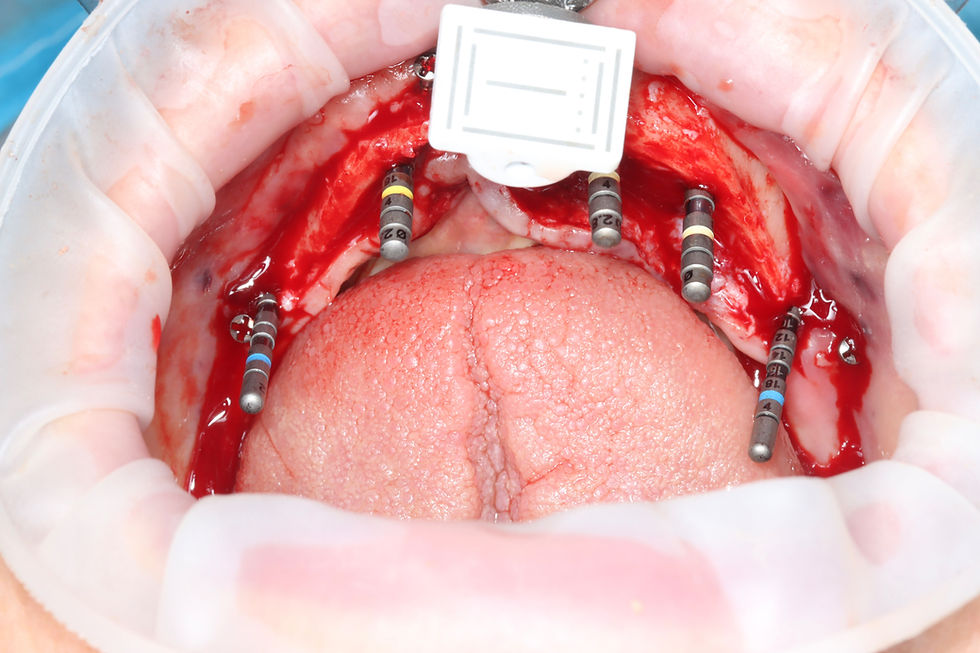
We anesthetized the patient with articaine 1:100,000 and performed a full-thickness mucoperiosteal flap. In the anterior esthetic zone, I usually try to avoid flap elevation in post-extraction implant cases because we know that full periosteal reflection may accelerate buccal bone resorption. However, in this case it was important to gain complete access for thorough debridement and cleaning of the infected area.
The extraction of tooth 13 was carried out very carefully, and we then initiated implant bed preparation. My protocol for upper canines is almost always the same. Before surgery, I carefully study the CBCT to evaluate the palatal wall thickness and define the ideal entry point for anchorage into basal bone. The spear drill initially enters at approximately 45 degrees toward the palatal wall, and then the angulation is progressively corrected toward the cingulum of the adjacent teeth.
After the initial preparation, I use a 2.0 mm drill following exactly the same trajectory. I always like to confirm the depth with a direction indicator pin, and in these situations I generally position the implant platform about 2 mm apical to the most coronal aspect of the buccal plate in order to create a more favorable emergence profile.
It is important to understand that although these implants are often placed very palatally to obtain stability, this does not mean that the prosthetic emergence will be compromised. Today we can manipulate prosthetic components and multi-unit abutments to redirect the emergence profile into a much more favorable position.
We then proceeded with the posterior implants.
In position 15 there were approximately 8 mm of residual bone height below the sinus, so I selected an 8 mm TLX NT implant. The preparation was performed using a 2.0 mm drill followed by a 2.8 mm drill, allowing a very gentle bicortical engagement through the sinus floor. The rationale in these situations is straightforward: minimally penetrate the sinus cortical floor in order to increase primary stability without excessively traumatizing the membrane.
The result was excellent:
Insertion torque of 77 Ncm in implant 13
Insertion torque of 76 Ncm in implant 15
Position 16 was far more challenging. We only had approximately 4 mm of residual bone, so we decided to use a first-generation 4 mm TLX implant. These implants have since evolved significantly in their apical design and are no longer identical to the original versions. Even so, we still achieved sufficient insertion torque to include it in the protocol.
We placed intermediate abutments on implants 13 and 15. On the 4 mm TLX implant we connected directly to the implant head, taking advantage of the tissue-level design and maintaining the prosthetic interface approximately 1–2 mm above the crestal bone.
Then came the digital workflow.
Scan bodies were placed and an intraoral scan was immediately performed and sent to Sofia. Sofia started designing the provisional PMMA bridge right away: CAD design, milling, and union of the prosthetic components. In this case we worked directly to the multi-unit abutments without additional interfaces, and in the 16 region we used a metallic interface directly connected to the TLX implant.
One extremely important detail in these immediate post-extraction cases is the palatal area. These implants are often highly engaged within the palatal wall, which may create difficulties both during abutment seating and during fabrication of the provisional restoration. It is essential for the laboratory technician to relieve the palatal aspect of the PMMA restoration appropriately to avoid compression against the palatal mucosa or even the palatal bone itself.
At the end of the procedure:
Final screw torque was set at 15 Ncm
Occlusion was meticulously adjusted
No centric or eccentric contacts were allowed
Because at the end of the day this is still an immediate loading protocol — and immediate loading lives or dies based on biomechanical control.
The patient was prescribed azithromycin, paracetamol 1 g as needed, and etoricoxib on the day of surgery. Now comes the most important biological phase: waiting. In these cases I usually prefer to allow approximately four months before delivering the definitive prosthesis. The patient will return in August for the final rehabilitation.
And in the middle of all this surgery, we still had time to discover that the patient’s husband works with bird tracking in England and later comes to Lisbon to verify whether the birds arrived safely. I immediately told him that birds should never travel by train… because by plane they clearly arrive faster.
Great case. Great team. Fantastic laboratory work by Sofia. And once again, proof that when we combine primary stability, digital planning, and strict occlusal control, we can transform potentially catastrophic situations into highly elegant rehabilitations.
Cheers Andre

Comments